Spinal Muscular Atrophy Type 1
June 15, 2011 in Chronic Illness - Disabilities
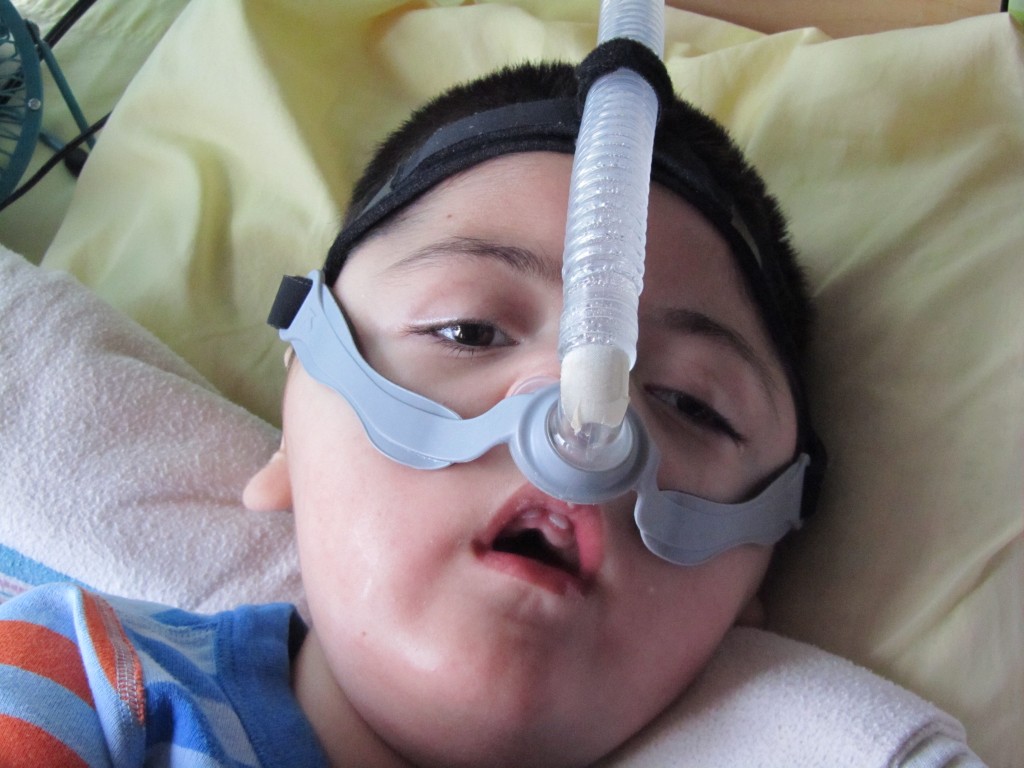 You’ve met my little friend Kian in a prior post, so I wanted to share his story. I started working with Kian in April of 2009. Kian lives with the disease SMA type 1 which is called Spinal Muscular Atrophy.
You’ve met my little friend Kian in a prior post, so I wanted to share his story. I started working with Kian in April of 2009. Kian lives with the disease SMA type 1 which is called Spinal Muscular Atrophy.
Families that go through such difficult times are incredible people as I have found in Kian’s.
I will start this journey by telling you about the SMA genetic challenge first. In future post I would like to share some of Kian’s abilities and the adventures of his daily life.
The info below is a short summary.
SMA is a genetic flaw sometimes called a mutation. SMA is more common than you may realize. I don’t wish to frighten you but to educate and make you aware of the signs and symptoms and pre-pregnancy testing that is available to couples.
*Spinal muscular atrophy (SMA), is the number one genetic killer of children under the age of two, is often fatal and destroys the nerves controlling voluntary muscle movement, which affects crawling, walking, head and neck control, and even swallowing and breathing.
*The nerve cells that control muscles are located in the spinal cord so this is how it gets the name Spinal Muscular Atrophy. The muscles stop recognizing signals from the spinal cord nerves and atrophy begins, which is the shrinking of muscles because they are inactive.
WHO IS AFFECTED
SMA is one of the most prevalent genetic disorders.
- One in every 6,000 babies is born with SMA.
- SMA can strike anyone of any age, race or gender.
- One in every 40 people carries the gene that causes SMA. The child of two carriers has a one in four chance of developing SMA.
- 7.5 million Americans are carriers.
There are 4 types of Spinal Muscular Atrophy
- Type 1, the most severe effects infants between birth and six months.
- Type 2, effects infants between 7 and18 months.
- Type 3, the least deadly effects children as early as 18 months and sometimes not until adolescence.
- Type 4, is an adult form where symptoms usually appear after 35 yr of age.
This post will focus on SMA1 which is the most severe. SMA1 used to take the life of a child by age 2, but with all the technology available today many children are surviving much longer even into their teens.
SMA1 is also called Werdnig-Hoffmann Disease. Children with SMA1 cannot sit without support.
2 areas that create some of the biggest challenges for SMA1 children are:
- Respiratory muscle weakness
- Swallowing muscle weakness
Respiratory problems cause a lack of oxygen the body needs, which can lead to chest infections, possible heart damage, respiratory failure and even death.
Belly breathing, which is a way to compensate for difficulty in breathing, is a sign you should tell your pediatrician.
Children with respiratory muscle weakness will eventually need help with secretions, so a suction machine is used. A small tube or catheter is placed down the throat as the machine sucks the secretions out. The suction machine is portable so will go with the child wherever he goes.
A cough machine helps bring up deep secretions and helps keep the lungs clear. A small respiratory mask is placed on the child for short intervals while the machine blows air in to expand the lungs and sucks out to bring up secretion. You and I rid ourselves of these secretions by coughing, hence the name Cough Assist. A portable one is in the process of creation.
Respiratory ventilation devices have helped some children live into their teens. The vent has the ability to be pre-set for the child’s specific breathing needs and is minimally invasive. The child wears a mask or just a nose/nasal piece to help with the breathing assistance he needs. The machines are portable so life is much easier than the old days of “the iron lung”, which was huge and immobile.
Swallowing muscle weakness is when a child cannot suck or swallow, so suctioning is required as described above and eventually they will receive their feeding via a gastronomy tube or G-tube. A G-tube feeds the child through a created hole to connect directly to the stomach. The child will have a little button (mickey button) on their stomach, which is a place to connect the bag of formula directly in to the stomach.
Infants with early signs of breathing, sucking and swallowing problems should be evaluated by their pediatrician.
Mental and emotional development and sensation are normal in SMA children.
Pre-pregnancy tests are available to see if couples are carriers, speak with your doctor before you become pregnant.
The information in this post was in part from FightSMA and Families of SMA, please check them out for more details for the care and treatment of children with SMA.
Updated 9/25/17 I started working with Kian in April of 2009. This is an introduction to SMA and I hope to tell you more of the adventures of Kian in his everyday world. Kian has a teacher and has some physical abilities. He enjoys moving his legs with the help of his slings. Kian has physical therapy, OT sessions and nurses who care for him around the clock. Kian has since receive a tracheostomy and his care is much easier for his nurses and family. He enjoys music, vocalizing, movies, crafts and attention from his little brothers, family and friends.
You may like: ♥ SMA child’s Tribute to his mom ♥ SMA child’s Tribute to his Dad ♥ Card making
Leave a Reply



